SHP2 (PTPN11) acts upstream of SOS1/2 to enable RAS activation. Allosteric SHP2 inhibitors (SHP2i) in the clinic prevent SHP2 activation, block proliferation of RTK- or cycling RAS mutant-driven cancers, and overcome “adaptive resistance.” To identify SHP2i resistance mechanisms, we performed genome-wide CRISPR/Cas9 knockout screens on two SHP2i-sensitive cell lines, recovering genes expected to cause resistance (NF1, PTEN, CDKN1B, LZTR1, and RASA2) and novel targets (INPPL1, MAP4K5, epigenetic modifiers). We screened 14 additional lines with a focused CRISPR library targeting common “hits” from the genome-wide screens. LZTR1 deletion conferred resistance in 12/14 lines, followed by MAP4K5 (8/14), SPRED2/STK40 (6/14), and INPPL1 (5/14). INPPL1, MAP4K5, or LZTR1 deletion reactivated ERK signaling. INPPL1-mediated sensitization to SHP2i required its NPXY motif but not lipid phosphatase activity. MAP4K5 acted upstream of MEK through a kinase-dependent target(s); LZTR1 had cell-dependent effects on RIT and RAS stability. INPPL1, MAP4K5, or LZTR1 deletion also conferred SHP2i resistance in vivo. Defining the SHP2i resistance landscape could suggest effective combination approaches.
J Exp Med (2023) 220 (5)
Intracellular oncoproteins can be inhibited with targeted therapy, but responses are not durable. Immune therapies can be curative, but most oncogene-driven tumors are unresponsive to these agents. Fragments of intracellular oncoproteins can act as neoantigens presented by the major histocompatibility complex (MHC) but recognizing minimal differences between oncoproteins and their normal counterparts is challenging. We have established a platform technology that exploits hapten-peptide conjugates generated by covalent inhibitors to create distinct neoantigens that selectively mark cancer cells. Using the FDA-approved covalent inhibitors sotorasib and osimertinib, we developed “HapImmuneTM” antibodies that bind to drug-peptide conjugate/MHC complexes but not to the free drugs. A HapImmuneTM-based bispecific T cell engager selectively and potently kills sotorasib-resistant lung cancer cells upon sotorasib treatment. Notably, it is effective against KRASG12C mutant cells with different HLA supertypes, HLA-A*02 and A*03/11, suggesting loosening of MHC restriction. Our strategy creates targetable neoantigens by design, unifying targeted and immune therapies.
Cancer Discov CD-22-1074
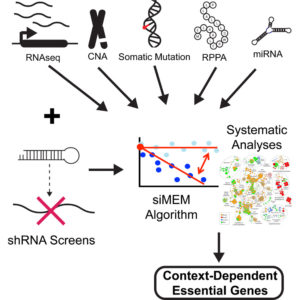
Abstract Resistance to targeted therapies is an important clinical problem in HER2-positive (HER2+) breast cancer. “Drug-tolerant persisters” (DTP), a subpopulation of cancer cells that survive via reversible, nongenetic mechanisms, are implicated in resistance to tyrosine kinase inhibitors (TKI) in other malignancies, but DTPs following HER2 TKI exposure have not been well characterized. We found that HER2 TKIs evoke DTPs with a luminal-like or a mesenchymal-like transcriptome. Lentiviral barcoding/single-cell RNA sequencing reveals that HER2+ breast cancer cells cycle stochastically through a “pre-DTP” state, characterized by a G0-like expression signature and enriched for diapause and/or senescence genes. Trajectory analysis/cell sorting shows that pre-DTPs preferentially yield DTPs upon HER2 TKI exposure. Cells with similar transcriptomes are present in HER2+ breast tumors and are associated with poor TKI response. Finally, biochemical experiments indicate that luminal-like DTPs survive via estrogen receptor-dependent induction of SGK3, leading to rewiring of the PI3K/AKT/mTORC1 pathway to enable AKT-independent mTORC1 activation. Significance DTPs are implicated in resistance to anticancer therapies, but their ontogeny and vulnerabilities remain unclear. We find that HER2 TKI-DTPs emerge from stochastically arising primed cells (“pre-DTPs”) that engage either of two distinct transcriptional programs upon TKI exposure. Our results provide new insights into DTP ontogeny and potential therapeutic vulnerabilities. This article is highlighted in the In This Issue feature, p. 873. Abstract Clinical trials of SHP2 inhibitors (SHP2i) alone and in various combinations are ongoing for multiple tumors with over-activation of the RAS/ERK pathway. SHP2 plays critical roles in normal cell signaling; hence, SHP2is could influence the tumor microenvironment. We found that SHP2i treatment depleted alveolar and M2-like macrophages and promoted B and T lymphocyte infiltration in Kras- and Egfr-mutant non-small cell lung cancer (NSCLC). However, treatment also increased intratumor gMDSCs via tumor-intrinsic, NF-kB-dependent production of CXCR2 ligands. Other RAS/ERK pathway inhibitors also induced CXCR2 ligands and gMDSC influx in mice, and CXCR2 ligands were induced in tumors from patients on KRASG12C-inhibitor trials. Combined SHP2(SHP099)/CXCR1/2(SX682) inhibition depleted a specific cluster of S100a8/9high gMDSCs, generated Klrg1+ CD8+ effector T cells with a strong cytotoxic phenotype but expressing the checkpoint receptor NKG2A, and enhanced survival in Kras-and Egfr-mutant models. Our results argue for testing RAS/ERK pathway/CXCR1/2/NKG2A inhibitor combinations in NSCLC patients. Significance Our study shows that inhibiting the SHP2/RAS/ERK pathway triggers NF-kB-dependent up-regulation of CXCR2 ligands and recruitment of S100A8high gMDSCs, which suppress T cells in NSCLC. Combining SHP2 and CXCR2 inhibitors blocks this gMDSC immigration, resulting in enhanced Th1 polarization, induction of CD8+ KLRG1+ effector T cells with high cytotoxic activity and improved survival in multiple NSCLC models. KRAS is the most frequently mutated oncogene in human cancer, and KRAS inhibition has been a longtime therapeutic goal. Recently, inhibitors (G12C-Is) that bind KRASG12C-GDP and react with Cys-12 were developed. Using new affinity reagents to monitor KRASG12C activation and inhibitor engagement, we found that, reflecting its action upstream of SOS1/2, SHP2 inhibitors (SHP2-Is) increased KRAS-GDP occupancy, enhancing G12C-I efficacy. SHP2-Is abrogated feedback signaling by multiple RTKs and blocked adaptive resistance to G12C-Is in vitro, in xenografts, and in syngeneic KRASG12C–mutant pancreatic ductal adenocarcinoma (PDAC) and non-small cell lung cancer (NSCLC) models. Biochemical analysis revealed enhanced suppression of ERK-, MYC-, anti-apoptotic-, and cell-cycle genes, and increased pro-apoptotic gene expression in tumors from combination-treated mice. SHP2-I/G12C-I also evoked favorable changes in the immune microenvironment, decreasing myeloid suppressor cells, increasing CD8+ T cells, and sensitizing tumors to PD-1 blockade. Experiments using cells expressing inhibitor-resistant SHP2 showed that SHP2 inhibition in PDAC cells is required for tumor regression and remodeling of the immune microenvironment, but also revealed direct inhibitory effects on angiogenesis resulting in decreased tumor vascularity. Our results demonstrate that SHP2-I/G12C-I combinations confer a substantial survival benefit in PDAC and NSCLC and identify additional combination strategies for enhancing the efficacy of G12C-Is. [preprint posted on bioRxiv 2020 May 31] SUMMARY The paucity of genetically informed, immune-competent tumor models impedes evaluation of conventional, targeted, and immune therapies. By engineering mouse fallopian tube (FT) organoids using lentiviral gene transduction and/or CRISPR/Cas9 mutagenesis, we generated multiple high grade serous ovarian carcinoma (HGSOC) models exhibiting mutational combinations seen in patients. Detailed analysis of homologous recombination (HR)-proficient (Tp53-/-;Ccne1OE;Akt2OE; KrasOE), HR-deficient (Tp53-/-;Brca1-/-;MycOE) and unclassified (Tp53-/-;Pten-/-;Nf1-/-) organoids revealed differences in in vitro properties and tumorigenicity. Tumorigenic organoids had variable sensitivity to HGSOC chemotherapeutics and evoked distinct immune microenvironments. These findings enabled development of a chemotherapy/immunotherapy regimen that yielded durable, T-cell dependent responses in Tp53-/-;Ccne1OE;Akt2OE;Kras HGSOC; by contrast, Tp53-/-;Pten-/-;Nf1-/- tumors failed to respond. Genotype-informed, syngeneic organoid models could provide an improved platform for rapid evaluation of tumor biology and therapeutics. HIGHLIGHTS Genetically Defined, Syngeneic Organoid Platform for Developing Combination Therapies for Ovarian Cancer The cell-of-origin of high grade serous ovarian carcinoma (HGSOC) remains controversial, with fallopian tube epithelium (FTE) and ovarian surface epithelium (OSE) both considered candidates. Here, by using genetically engineered mouse models and organoids, we assessed the tumor-forming properties of FTE and OSE harboring the same oncogenic abnormalities. Combined RB family inactivation and Tp53 mutation in Pax8 + FTE caused Serous Tubal Intraepithelial Carcinoma (STIC), which metastasized rapidly to the ovarian surface. These events were recapitulated by orthotopic injection of mutant FTE organoids. Engineering the same genetic lesions into Lgr5 + OSE or OSE-derived organoids also caused metastatic HGSOC, although with longer latency and lower penetrance. FTE- and OSE-derived tumors had distinct transcriptomes, and comparative transcriptomics and genomics suggest that human HGSOC arises from both cell types. Finally, FTE- and OSE-derived organoids exhibited differential chemosensitivity. Our results comport with a dualistic origin for HGSOC and suggest that the cell-of-origin might influence therapeutic response. Both fallopian tube and ovarian surface epithelium are cells-of-origin for high-grade serous ovarian carcinoma Nat Commun 10, 5367 (2019) The RAS/ERK MAP kinase pathway is aberrantly activated in a large percentage of human cancers, and promotes malignant behavior. Inhibitors of MEK, one of the key intermediates in this pathway, have had limited utility in the clinic, often due to the rapid development of “intrinsic resistance.” Intrinsic resistance is due to up regulation of multiple growth factor receptors and their ligands, and previous work by the lab and by others has shown that is required for RAS activation by these receptors. Here we found that combining MEK and SHP2 inhibitors shows broad efficacy against a wide range of malignancies, and also that SHP2 inhibitors as single agents can antagonize certain types of RAS mutations (fast cycling mutants). SHP2 Inhibition Prevents Adaptive Resistance to MEK Inhibitors in Multiple Cancer Models. Mutations of one copy of TET2, whose protein product promotes DNA (and RNA) hydroxymethylation (and eventually, DNA and RNA de-methylation, are commonly associated with myelodyspastic syndromes (MDS) and acute myeloid leukemia, among other hematopoietic neoplasms. Previous work had suggested that Vitamin C, an essential co-factor of TET2, can promote TET2 activation as well. We found that high dose vitamin C, acting via residual TET2 and TET3, had potent anti-neoplastic effects in mouse and human models of MDS/AML. Molecular analysis confirmed that this treatment promotes demethylation of key leukemia-associated genes, including base excision repair genes. The latter result suggested that PARP inhibitors might further increase Vitamin C efficacy, which we also demonstrated. Vitamin C in Stem Cell Reprogramming and Cancer This paper presented the largest (at the time) collection of genome wide shRNA screens of human breast cancer lines, all linked to genomic (mutations, copy number variants, RNAseq, miRNAs) information and RPPA, along with detailed informatics analysis that suggests functional classifications of cancer vulnerabilities. Functional Genomic Landscape of Human Breast Cancer Drivers, Vulnerabilities, and ResistanceCreating MHC-restricted neoantigens with covalent inhibitors that can be targeted by immune therapy
Ontogeny and Vulnerabilities of Drug-Tolerant Persisters in HER2+ Breast Cancer
Combined Inhibition of SHP2 and CXCR1/2 Promotes Anti-Tumor T Cell Response in NSCLC
SHP2 Inhibition Abrogates Adaptive Resistance to KRASG12C-Inhibition and Remodels the Tumor Microenvironment of KRAS-Mutant Tumors
ABSTRACT
Genetically Defined, Syngeneic Organoid Platform for Developing Combination Therapies for Ovarian Cancer
[preprint posted on bioRxiv 2020 Apr 07]Both fallopian tube and ovarian surface epithelium are cells-of-origin for high-grade serous ovarian carcinoma
SHP2 Inhibition Prevents Adaptive Resistance to MEK Inhibitors in Multiple Cancer Models
Cancer Discov. 2018 Oct;8(10):1237-1249.Vitamin C in Stem Cell Reprogramming and Cancer
Trends Cell Biol. 2018 Sep;28(9):698-708.
Functional Genomic Landscape of Human Breast Cancer Drivers, Vulnerabilities, and Resistance
Cell. 2016 Jan 14;164(1-2):293-309.